At the beginning of the 20th century, allergies were uncommon and even seen as rare. Today, allergies, including environmental, food, allergic asthma, and eczema, are the most common chronic diseases experienced by people around the world.¹ In total, 120 million Americans, or 1 in 3, suffer from allergies.
While allergies are on the rise, their impact on our lives is not fully appreciated by the general population. Allergies have been linked to a 14x higher rate of migraines, a 6x higher rate of anxiety, and a 3x higher rate of depression.[²][³][⁴][⁵] In addition, over 50 million Americans suffer from environmental allergies, but many are unaware of the connection that environmental allergies have to asthma and other conditions. For example, the Asthma and Allergy Foundation of America found that 81% of the general population did not know that the most common form of asthma is allergic asthma or that asthma can be triggered by an environmental allergy.
According to the World Allergy Organization, allergic diseases represent a significant health problem globally. Allergies and their symptoms evolve as environments continue to change, but some of the most common allergy symptoms include⁶:
- Sneezing and an itchy, runny, or blocked nose
- Itchy, red, watering eyes
- Wheezing, chest tightness, shortness of breath, and a cough
- Hives
- Swollen lips, tongue, eyes, or face
- Anaphylaxis
There are many theories about why environmental allergies have become more prevalent with time. One theory is that rising global temperatures and carbon dioxide emissions have caused more rapid plant growth, creating more pollen. A second theory is that our microbiomes (the community of microorganisms that exists in and on our bodies) have changed with time, making us more likely to develop allergies.
Pollen is here to stay
Climate change may look different depending on where you’re located in the world. But there aren’t many environments that are immune to the effects of warmer temperatures. The combination of both higher temperatures and CO2 emissions allows plants to grow in more aggressive ways, which can produce more pollen than normal.⁷ And the more pollen there is, the more likely it is we’ll experience allergies.⁸
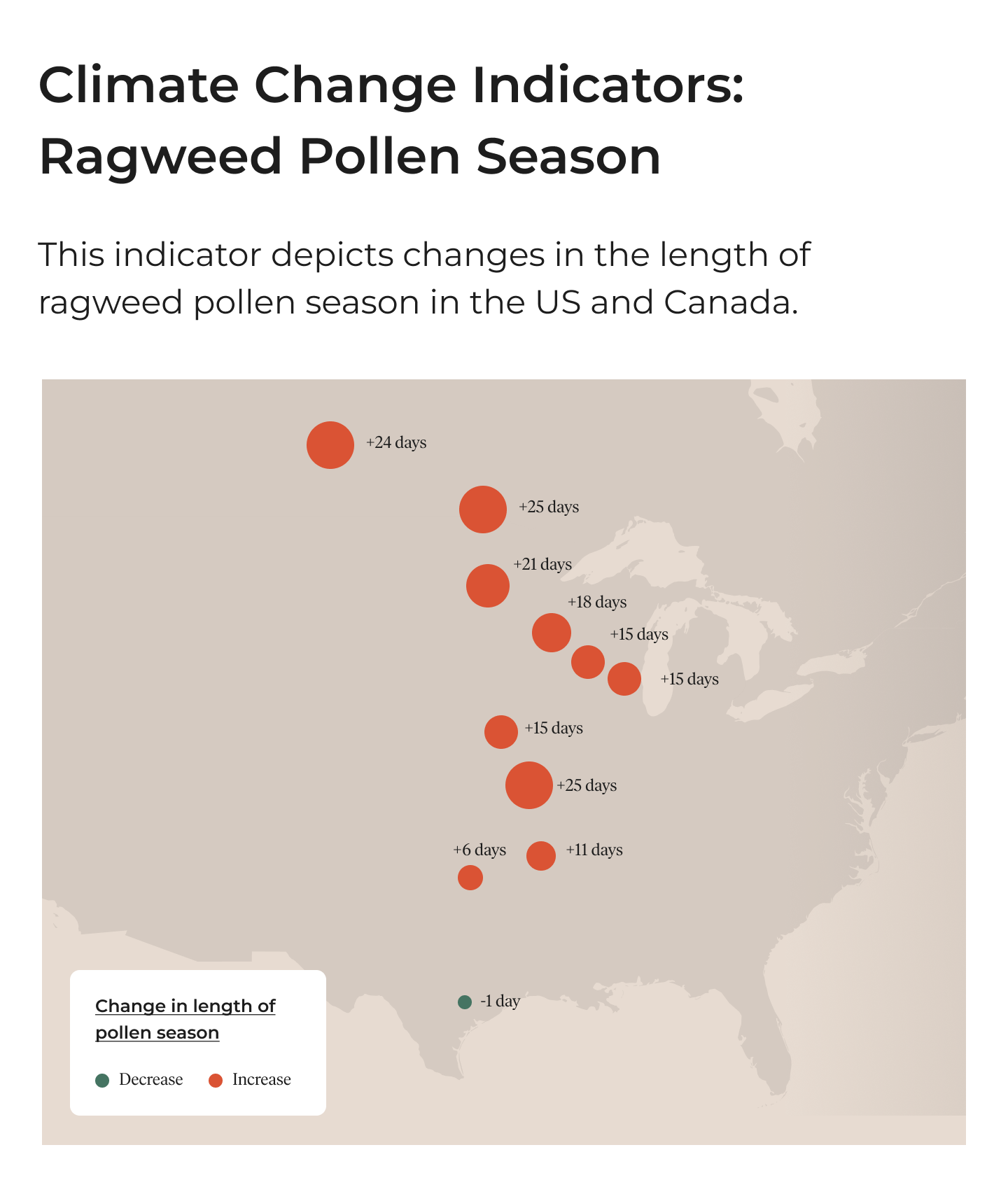
The figure above shows that areas in the north are entering frost season later than usual, which correlates to the increase in pollen season. More specifically, ragweed pollen season has actually gotten longer since 1995 in over 90% of locations it’s been studied (see figure). In Winnipeg, Manitoba alone, it is 25 days longer, and this trend is only more pronounced in regions further north.⁹
Allergic reactions are the body’s immune system responding to a substance that is normally harmless, like the proteins that coat pollen. The severity of a reaction depends on three connected factors:
- How much pollen a particular plant releases into the air
- The amount of exposure an individual has to the pollen
- The capacity the pollen has to cause a reaction (otherwise known as allergenicity)
Ragweed is one example of an allergen that ranks high on all three factors, making it the perfect trigger for pollen allergy sufferers.¹⁰
Early exposure to microbes and the body’s inner environment
What lives on our skin and in our bodies is a direct reflection of how and where we live. For example, a modern-day Western lifestyle includes a specific diet and environment, which creates a certain human microbiota (all the bacteria that live within and on our bodies). That microbiota is going to be distinct from, say, the microbiota of our parents’ generations. Some doctors think that the increase in allergies has to do with less exposure to certain parasites and bacteria that might have previously protected us. A peer-reviewed article published in the Journal of Allergy and Clinical Immunology refers to this phenomenon as the ‘old friends hypothesis’—that humans need to be exposed to symbiotic microbes (aka good bacteria) during childhood in order to properly develop adaptive immunity.¹¹
There is preliminary evidence from recent studies around the ways we adapt to environmental microbes and how that relates to allergies. For example, one study found that infants who were born by cesarean delivery had increased sensitivity to allergies due to delays in the microbiota development of their intestines, as opposed to infants born by vaginal birth which caused them to pick up more good bacteria during the birthing process.[¹²][¹³]
According to the Practall Consensus Report, researchers are beginning to see a connection between the bacteria in our respiratory and gastrointestinal tracts, and how that affects our likelihood of having asthma and other allergies. More specifically, the diversity and composition of these bacteria can increase or decrease our risk of developing allergies.¹⁴
Taking lots of antibiotics early on in life can also increase allergy risk because of the ways antibiotics behave in the body. Antibiotics don’t discriminate between good and bad bacteria, they simply kill them all. Good bacteria are necessary for survival and can help decrease a person’s risk for allergies.
The future of allergy testing and treatment
While the nature of allergies has and will continue to evolve, there is hope for allergy sufferers. Technological advances in science and medicine have created viable solutions for many people who experience allergies through immunotherapy, which treats the root cause of the allergy rather than simply managing the symptoms.
Citations:
¹ Ring, J et al. “Davos declaration: allergy as a global problem.” Allergy vol. 67,2 (2012): 141-3. doi:10.1111/j.1398-9995.2011.02770.x
² Aamodt, Anne H et al. “Is headache related to asthma, hay fever, and chronic bronchitis? The Head-HUNT Study.” Headache vol. 47,2 (2007): 204-12. doi:10.1111/j.1526-4610.2006.00597.x
³ Ku, M. J., et al. “The Prevalence of Migraine Headaches in Patients with Allergic Rhinitis.” Journal of Allergy and Clinical Immunology, vol. 115, no. 2, Feb. 2005, p. S197.
⁴ Ozturk, Ayhan et al. “Frequency of migraine in patients with allergic rhinitis.” Pakistan journal of medical sciences vol. 29,2 (2013): 528-31. doi:10.12669/pjms.292.3148
⁵ Saberi, Alia et al. “Association between allergic rhinitis and migraine.” Journal of research in medical sciences: the official journal of Isfahan University of Medical Sciences vol. 17,6 (2012): 508-12.
⁶ Papadopoulos, Nikolaos G et al. “Research needs in allergy: an EAACI position paper, in collaboration with EFA.” Clinical and translational allergy vol. 2,1 21. 2 Nov. 2012, doi:10.1186/2045-7022-2-21
⁷ Ziska, Lewis H, and Paul J Beggs. “Anthropogenic climate change and allergen exposure: The role of plant biology.” The Journal of allergy and clinical immunology vol. 129,1 (2012): 27-32. doi:10.1016/j.jaci.2011.10.032
⁸ Anderegg, William R. L., et al. “Anthropogenic Climate Change Is Worsening North American Pollen Seasons.” Proceedings of the National Academy of Sciences, vol. 118, no. 7, 8 Feb. 2021, p. e2013284118, 10.1073/pnas.2013284118.
⁹ Ziska, Lewis, et al. “Recent Warming by Latitude Associated with Increased Length of Ragweed Pollen Season in Central North America.” Proceedings of the National Academy of Sciences, vol. 108, no. 10, Mar. 2011, pp. 4248–51.
¹⁰ Schmidt, Charles W. “Pollen Overload: Seasonal Allergies in a Changing Climate.” Environmental health perspectives vol. 124,4 (2016): A70-5. doi:10.1289/ehp.124-A70
¹¹ Bunyavanich, Supinda, and M. Cecilia Berin. “Food Allergy and the Microbiome: Current Understandings and Future Directions.” The Journal of Allergy and Clinical Immunology, vol. 144, no. 6, Dec. 2019, pp. 1468–77.
¹² Bunyavanich, Supinda, and M. Cecilia Berin. “Food Allergy and the Microbiome: Current Understandings and Future Directions.” The Journal of Allergy and Clinical Immunology, vol. 144, no. 6, Dec. 2019, pp. 1468–77.
¹³ Eggesbø, Merete, et al. “Is Delivery by Cesarean Section a Risk Factor for Food Allergy?” Journal of Allergy and Clinical Immunology, vol. 112, no. 2, Aug. 2003, pp. 420–26.
¹⁴ J. Huang, Yvonne, et al. "The Microbiome in Allergic Disease: Current Understanding and Future Opportunities—2017 PRACTALL Document of the American Academy of Allergy, Asthma & Immunology and the European Academy of Allergy and Clinical Immunology." Elsevier Inc, 17 Feb. 2017.





